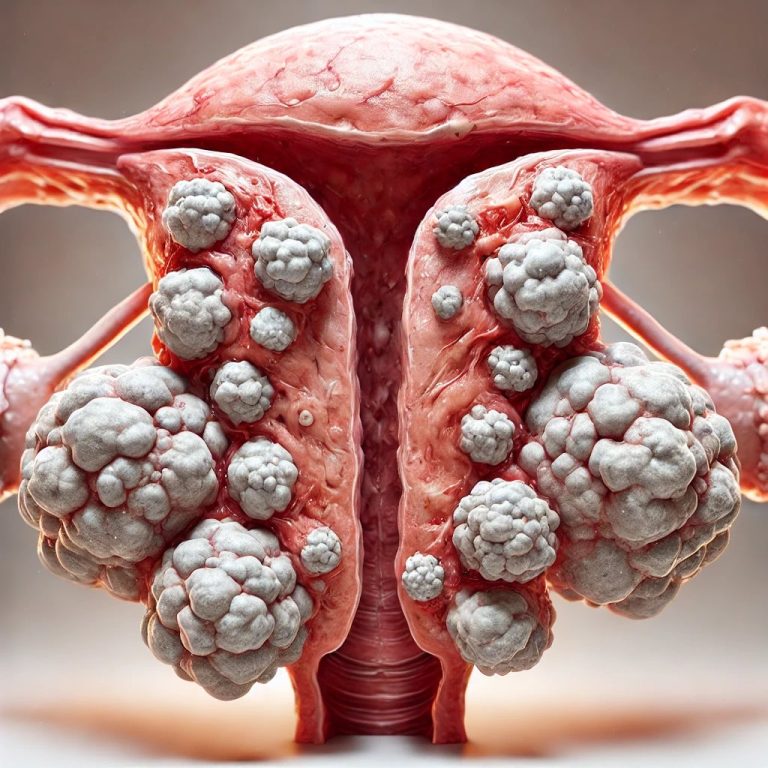
The reproductive organs are the key biological components that differentiate women from men.
The organs include the uterus, ovaries, fallopian tubes, cervix, and vagina, which function together to enable reproduction, pregnancy, and childbirth.
However, one of the most significant reproductive health challenges affecting the reproductive organs of women globally, particularly those of African descent, is uterine fibroids.
Uterine fibroids, or leiomyomas, are non-cancerous growths of the uterus that often appear during the childbearing years.
While these muscular tumours are rarely life-threatening, the World Health Organisation (WHO) says they are a major public health issue for women of reproductive age.
According to WHO, fibroids are non-cancerous tumours that grow in the uterus and are made up of muscle and fibrous tissue.
Treatment ranges from surgery to non-invasive procedures and medications, depending on their impact on the individual.
Research over the years has shown that African women have the highest prevalence of uterine fibroids in the world, where the condition is associated with significant morbidity, economic and health system costs, and occasional mortality.
According to available research, the prevalence of uterine fibroids in Nigeria is significantly high, ranging from 17.9 per cent to 26 per cent.
Studies indicate that fibroids account for a substantial portion of gynaecological cases in Nigeria, representing 3.2 per cent to 7.8 per cent of all gynaecological issues and a large majority of hysterectomy cases.
While many have successfully undergone fibroid surgery to improve their quality of life or increase their chances of having children, others have died due to complications resulting from the same medical procedure.
Mr Samuel Eze, who lost his wife in 2023 due to complications from fibroid surgery, narrated how she bled to death, noting that all efforts by the medical team to save her in a hospital in the Ikotun area of Lagos failed.
Eze noted that his late wife, who died in her forties, had several miscarriages that were attributed to fibroids, and she was advised to undergo surgery to increase her chances of giving birth.
“If I knew my wife would not survive the surgery, we wouldn’t have gone ahead with it, but she insisted on having the surgery to have her own children,” he said.
These and many more are the ordeals of families still grieving the deaths of their loved ones who died during or after undergoing fibroid surgery.
Some common complications that could occur from surgery range from haemorrhage, injury to surrounding organs, anaesthesia-related risks, and infections, said Prof. Oliver Ezechi, Director of Research at the Nigerian Institute of Medical Research (NIMR).
However, Ezechi, who is also a professor of Maternal, Reproductive and Child Health at Lead City University in Ibadan, noted that pre-operative assessment before surgery was key to identifying any possible complications likely to arise during surgery.
He noted that some of the reasons women opted for fibroid surgery were to improve their quality of life and increase their chances of becoming mothers, heavy bleeding, severe pain, suspicion of malignancy, fertility issues, among others.
“Fibroids are non-cancerous tumours of the womb that can significantly impact women’s reproductive health, causing symptoms such as heavy menstrual bleeding, pelvic pain, and pressure on surrounding organs.
“The presence of fibroids can also affect fertility and pregnancy outcomes, leading to complications such as miscarriage or preterm birth.
“It is a major cause of ill health and occasional death following surgery in incompetent hands,” he said.
However, Ezechi noted that mortality from fibroid procedures could be averted through advanced treatments.
The expert explained that, apart from surgery, other advanced treatments for fibroids include hormonal therapies (such as GnRH agonists) to help shrink fibroids and manage symptoms, and uterine artery embolisation, which cuts off blood supply to fibroids, causing them to shrink.
“Others are MRI-guided focused ultrasound, a non-invasive treatment that uses ultrasound to destroy fibroid tissue, and endometrial ablation, a procedure that removes the lining of the uterus to reduce heavy bleeding caused by fibroids,” he said.
Ezechi emphasised that each treatment option has its benefits and risks, adding that the choice depends on individual health needs and preferences.
A consultant obstetrician and gynaecologist, Dr James Odofin, explained that most complications that occurred during fibroid surgery might not be as a result of the surgical procedure itself but could also be caused by other medical conditions, hence the need for thorough evaluation before surgery.
Odofin said: “Before any surgical procedure, a patient needs to be thoroughly evaluated to know if the person has any underlying health issues that should be addressed before going for surgery.
“For example, a patient with hypertension or a chronic medical illness that is not well optimised before surgery, no matter how simple the procedure is, can have complications aggravated by surgical techniques or anaesthetic agents.
“With just basic tests, an emergency caesarean section can be done to save a mother and child, but an elective surgery such as fibroid surgery requires certain investigations called effective pre-operative work-up of the patient.”
The consultant, who works at the Federal Medical Centre, Ebute Metta, said aversion to surgery in the country and on the continent at large prevents patients from seeking timely medical help, adding that patients usually present late.
As such, he urged that to address most complications associated with fibroid surgery, patients need to be well informed and seek prompt medical attention from competent specialists.
He also urged the government to increase access to quality care, as well as ensure the availability of advanced treatment options to reduce mortality during such procedures.